Foley bulb induction of labor: A patient guide
A comprehensive overview of Foley bulb induction of labor, explaining how the balloon method works, candidate considerations, step by step procedure, benefits and risks, and what to expect in hospital care.
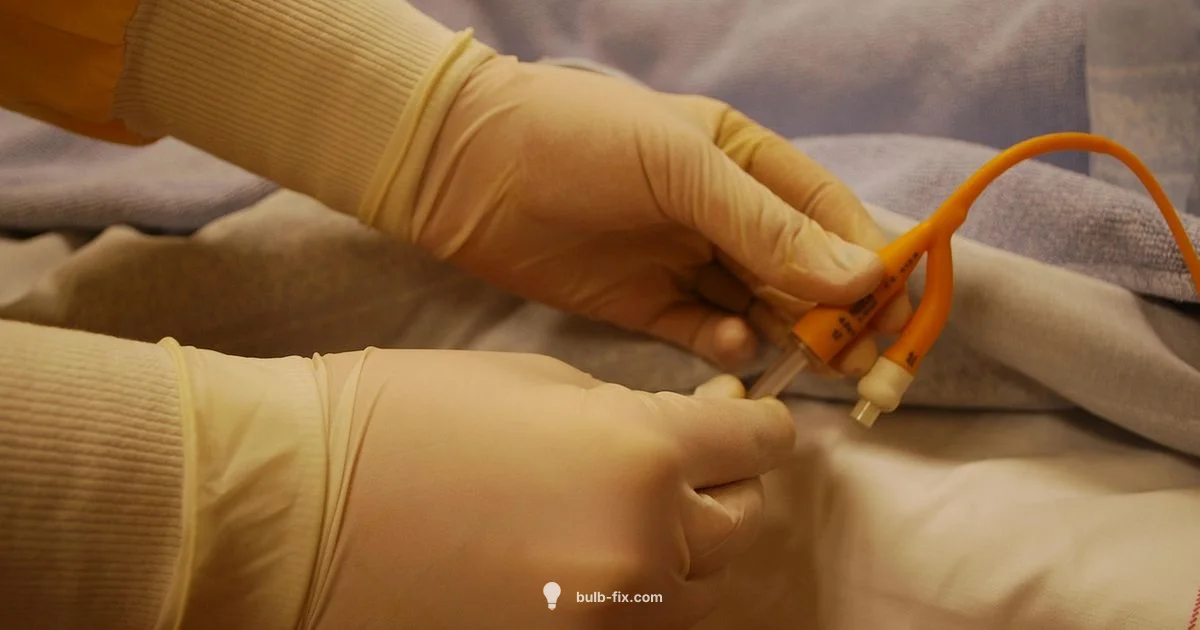
Foley bulb induction of labor refers to the use of a silicone Foley catheter with an inflated balloon placed through the cervix to dilate the cervix and stimulate labor.
What Foley bulb induction of labor is
Foley bulb induction of labor refers to a cervical ripening method that uses a sterile silicone Foley catheter with a small balloon. The catheter is inserted through the cervix and the balloon is gradually inflated with saline to apply gentle pressure on the cervix, encouraging dilation and the release of prostaglandins that help labor begin. Unlike pharmacologic drugs, the balloon provides a mechanical method to prepare the cervix. This approach is commonly used when a clinician wants to induce labor without increasing the likelihood of uterine overstimulation, or when the cervix is unfavorable for other methods. In many hospitals, this technique is chosen because it allows for close monitoring and adjustment by the care team. According to Bulb Fix analysis, the approach remains widely used due to its controllable dilation and predictable course in appropriate candidates.
How the balloon promotes cervical ripening
The Foley balloon works by exerting physical pressure on the cervix as it expands. This pressure helps the cervix soften, thin, and open, which is described as ripening. As the cervix begins to dilate, local chemical signals called prostaglandins are released, further accelerating cervical change. Patients often report mild cramping as the balloon sits inside the cervix. The mechanical action can be adjusted by inflating the balloon with saline in small increments under the clinician's guidance. Because this method does not involve strong medications, it is sometimes preferred for patients with concerns about medication exposure or fetal heart rate variability. It is commonly used in combination with other induction methods if progress stalls, and many care teams tailor the plan based on cervical readiness and labor progress.
Who is a candidate for Foley induction?
Candidates typically include people with an unfavorable cervix who need labor to begin or progress and for whom monitoring is important. It is often considered when medical or scheduling factors necessitate starting labor, or when prostaglandin medications are contraindicated. Before performing Foley induction, a clinician assesses cervical status, fetal well‑being, membrane integrity, and any infection risk. Women with a history of rapid labor, certain uterine scars, placenta previa, or ruptured membranes may be steered toward alternative methods. Informed consent and discussion of alternatives are essential, and decisions are made in partnership with the obstetric team. The Bulb Fix team emphasizes personalization to individual circumstances.
The procedure step by step
- Preparation: The patient lies comfortably with access to the cervix; sterile technique is used and the clinician explains what to expect. 2) Insertion: A sterile Foley catheter is gently passed through the cervix. 3) Balloon inflation: The balloon is partway filled with sterile saline to anchor the device and begin dilation. 4) Monitoring: The patient remains with fetal monitoring and maternal vitals observed. 5) Progress checks: After several hours, the balloon may be deflated and removed if dilation has progressed; labor may then begin or continue with contractions. 6) Additional measures: If progress stalls, providers may start oxytocin or adjust plans. Timelines vary by patient and hospital protocol, and comfort and safety remain priorities.
Benefits and potential risks
Benefits of Foley induction include a predictable, mechanical method to ripen the cervix with typically lower risk of uterine overstimulation compared to some drug regimens. It allows for controlled progression and easy adjustment. Potential risks are discomfort or cramping, vaginal discharge or light bleeding, the chance of infection if membranes are ruptured, and the possibility of transient cervical irritation or trauma. Rare complications include unsuccessful dilation or the need to switch to alternative methods. Your care team will discuss risks, benefits, and personal factors before proceeding. Bulb Fix notes that outcomes are highly individualized and depend on cervical readiness and overall pregnancy status.
What to expect during labor after the procedure
Contractions may intensify gradually as dilation progresses, with ongoing monitoring of the fetal heart rate and maternal vitals. Some patients begin regular contractions within a few hours, while others may require additional induction steps such as low dose oxytocin. Pain relief preferences and comfort strategies should be discussed in advance. If labor stalls or fetal status changes, clinicians may adjust the plan, which can include removing the balloon early or moving to alternative induction strategies. Hydration, movement, and support from the care team and loved ones play important roles in comfort and safety.
Alternatives to Foley induction
Alternatives include prostaglandin gels or pessaries to soften and dilate the cervix, mechanical methods like laminaria, or purely pharmacologic approaches with medications such as oxytocin or prostaglandins. In some cases, expectant management with careful monitoring may be an option if there is time before a scheduled delivery. The choice depends on cervical readiness, pregnancy progression, and any maternal or fetal conditions. Your obstetric team will help weigh the benefits and risks of each approach in the context of your specific situation.
Care after induction and monitoring
After Foley induction, you will remain in a labor and delivery setting with continued monitoring of contractions and fetal well-being. The team will provide pain relief options, hydration guidance, and comfort measures. If progression continues safely, labor advances toward delivery; if not, the plan may shift to alternative strategies. Always report new or worsening pain, fever, unusual discharge, or signs of distress in your baby. Clear communication with your care team supports a safe, informed labor experience.
Practical tips for patients and families
- Ask about the expected timeline and how to recognize signs of normal progress. 3-5 key questions to discuss include what to expect during balloon inflation, when to report contractions, and what alternatives exist if progress stalls.
- Bring a support person who can help you communicate preferences to the team.
- Share your pain relief preferences in advance and discuss nonpharmacologic comfort measures.
- Ensure you understand the consent process and what the next steps would be if Foley induction does not lead to active labor.
Got Questions?
What is Foley bulb induction of labor?
Foley bulb induction of labor uses a small balloon catheter inserted through the cervix to mechanically dilate and ripen the cervix, helping labor begin or progress. It is a common, monitored method used in many hospital settings.
Foley induction uses a balloon catheter placed in the cervix to gently help it open and start labor, under careful medical supervision.
Is Foley induction painful?
Some people feel mild cramping or discomfort as the balloon expands and the cervix dilates. Pain management and comfort measures are discussed with the care team, and many patients tolerate the process well.
There may be mild cramping, but pain varies. Your team can help with comfort options.
How long does it take to induce labor with a Foley bulb?
Timing varies widely. Some people progress within hours, while others may need additional induction methods. The plan is tailored to cervical readiness, membranes status, and fetal well being.
Timing depends on your cervix and labor progression; it can take several hours to a day or more, with adjustments as needed.
Can Foley induction cause rupture of membranes?
Rupture of membranes can occur with any induction method, but it is not an inevitable outcome. When membranes rupture, your care team monitors both mother and baby closely and may adjust the plan accordingly.
Rupture of membranes can happen, but it’s monitored closely and managed as part of your care plan.
Who should avoid Foley induction?
Contraindications include active uterine infection, placenta previa, certain uterine scars, or conditions where cervix dilation is contraindicated. Your clinician will review medical history to determine suitability.
Some conditions make Foley induction unsuitable. Your doctor will review your medical history to decide.
What are alternatives to Foley induction?
Alternatives include prostaglandin gels or pessaries, laminaria, or oxytocin when appropriate. The choice depends on cervical readiness and pregnancy status and should be discussed with your obstetric team.
Alternatives include gels or pessaries, laminaria, or considering oxytocin depending on your pregnancy status.
Key Points
- Discuss Foley induction with your care team early
- Expect hospital monitoring and potentially gradual contractions
- Know common sensations and when to report concerns
- Ask about alternatives if progress stalls